Patent Foramen Ovale (PFO) & Atrial Septal Defect Closure
Patent foramen ovale
A patent foramen ovale (PFO) is a residual defect or hole between the 2 upper chambers of the heart (atria) that is relatively common. The foetal foramen ovale is a connection between the right and left atria of the heart that allows oxygenated blood from the placenta to bypass the non-functioning lungs and directly enter the left side of the heart, where it can be pumped around the foetal body. This defect spontaneously closes after birth in most people but remains open or patent in a minority (25%). A PFO may cause no problems throughout a person’s life and most people are unaware that they even have one. However, it may cause problems in some people.
“My utmost priority is to provide the highest quality and most up-to-date cardiovascular care to all my patients. I aim to achieve this using a holistic approach in a personable and empathetic atmosphere, while taking into consideration each individual patient’s own wishes and hopes for their medical care.”
PFO has been linked to stroke, transient ischaemic attacks, heart attacks, migraine with aura, peripheral embolism, shortness of breath (platypnea orthodeoxia), decompression sickness in divers and high-altitude sickness. There are certain anatomical features that make some PFOs higher risk than others. Dangerous PFOs are ones that are large, have an atrial septal aneurysm, a Eustachian valve or a promiant Chiari network. This features can be diagnosed using a transoesophageal echocardiogram.
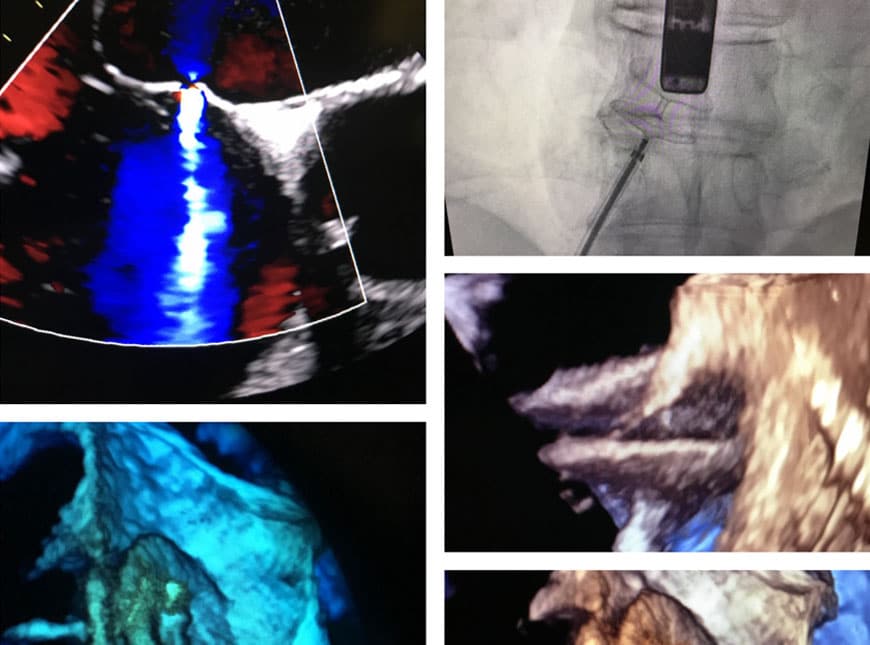
A PFO can be closed using an umbrella device. The procedure is performed under general anaesthesia or conscious sedation. After a small incision is made in the groin, a long think tube called a catheter is inserted into a vein in the leg. The PFO closure device is then guided through the catheter to the heart and once there it is implanted. A couple of months after the PFO closure device is implanted, tissue begins to cover the device. You will generally be discharged from hospital within 24 hours of the procedure.
ASD
There are 3 types of atrial septal defects i.e. ostium primum ASD, ostium secundum ASD and sinus venosus ASD. Ostium secundum ASDs are the most common type and occur during foetal development when a part of the atrial septum fails to close completely when the heart is developing. This can lead to problems later in life such as heart arrhythmias (atrial fibrillation) and elevated pressure in the blood vessels supplying the lungs (pulmonary hypertension). It can also lead to a stroke (paradoxical embolism). An ostium secundum ASD can be treated using a minimally invasive procedure performed through the groin using an umbrella closure device similar to the closure of a PFO.










